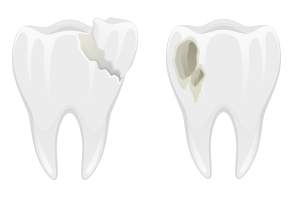
Problems that begin as tiny lines in enamel can let bacteria reach dentin and pulp, increasing sensitivity, decay, and risk of infection or sudden fracture; if you ignore them, your tooth may require root canal or extraction. You should have small cracks evaluated promptly so your dentist can monitor, stabilize, or restore the tooth and prevent more extensive, costly treatment later.
Understanding Tooth Structure
Your tooth is a layered organ where each layer affects how a small crack progresses: enamel shields the crown, dentin transmits forces and sensations, pulp houses nerves and blood vessels, and supporting tissues anchor the root. Enamel is the hardest tissue in your body but is only 1-2.5 mm thick on biting surfaces, so even superficial damage can expose deeper, more vulnerable layers and accelerate breakdown if untreated.
Composition of Teeth
You rely on four primary components: enamel (about 96% mineral hydroxyapatite by weight), dentin (roughly 70% mineral with tubules that carry sensations), pulp (nerves, blood supply and immune cells), cementum (covers root and helps anchor fibers), and the periodontal ligament (a 0.15-0.38 mm shock-absorbing connective layer). These proportions determine how a crack transmits force and pain to your nerve.
| Enamel | ~96% mineral, 1-2.5 mm thick on cusps, resists wear but doesn’t heal |
| Dentin | ~70% mineral, contains tubules that amplify sensitivity and crack propagation |
| Pulp | Soft tissue with nerves/blood vessels; infection here often requires root canal |
| Cementum | Thin root covering that anchors periodontal ligament fibers |
| Periodontal Ligament | Connective tissue ~0.2-0.3 mm wide; absorbs occlusal forces |
Types of Tooth Cracks
You commonly encounter five categories: craze lines (superficial, cosmetic), fractured cusp (often around fillings), cracked tooth (extends to pulp border), split tooth (separable segments, often untreatable), and vertical root fracture (starts below gumline). Biting hard objects, bruxism, or large restorations increase your risk; molars are the most affected due to higher occlusal loads.
- Pain on chewing that comes and goes, often when releasing bite
- Sharp sensitivity to cold or sweet that lingers inconsistently
- Visible lines on enamel or pieces that feel rough
- Swelling or tenderness around a specific tooth or gum
- Any time you notice intermittent bite pain, have it evaluated promptly
| Craze Lines | Superficial enamel only; cosmetic concern; no treatment usually required |
| Fractured Cusp | Often near large restorations; may need crown or onlay to restore strength |
| Cracked Tooth | Vertical crack into dentin/pulp borderline; RCT and crown frequently used |
| Split Tooth | Full-thickness separation; extraction or segment removal often required |
| Vertical Root Fracture | Starts below gumline; may cause localized bone loss and often extraction |
You should expect different diagnostic approaches: bite tests and transillumination reveal cracks in 60-80% of symptomatic cases, radiographs detect only a minority of vertical fractures, and CBCT can clarify uncertain cases. In one clinical series, timely placement of a full-coverage crown after diagnosing a cracked tooth improved survival to over 80% at three years; delaying care increased risk of pulp infection and tooth loss.
- Use a soft-bristled brush and avoid hard foods to limit propagation
- Nightguard therapy lowers peak occlusal forces in bruxers, reducing progression
- Timely restoration of large fillings distributes forces more evenly
- Discuss restorative options and prognosis with your dentist based on imaging
- Any unexplained, intermittent bite pain warrants prompt dental assessment
| Diagnosis Tool | Bite tests, transillumination, periapical radiograph, CBCT for unclear cases |
| Conservative Treatment | Bonded onlay or crown to splint tooth and prevent propagation |
| Endodontic Need | Cracks reaching pulp often require root canal before restoration |
| When Extraction | Split tooth or vertical root fracture with bone loss usually non-restorable |
| Prognosis Factors | Crack depth, location (crown vs root), time to treatment, and occlusal forces |
Causes of Small Tooth Cracks
Dietary Factors
Frequent exposure to acids and hard foods weakens enamel and initiates microcracks: cola and sports drinks (pH around 2.5-3) dissolve mineral content, while citrus and wine repeatedly lower oral pH below the 5.5 enamel threshold; grazing or sipping across hours prevents saliva from restoring balance, and biting hard items like unpopped popcorn kernels concentrates force on tiny flaws.
- Acidic beverages (colas, energy drinks) often have pH < 3, increasing demineralization.
- Repeated acid exposure reduces enamel hardness-studies show measurable softening after days of frequent acid contact.
- Assume that combining frequent acid exposure with chewing hard objects multiplies the chance that microcracks form and propagate.
Dental Habits
Your brushing technique and daily habits often create or worsen tiny fractures: aggressive horizontal strokes with a hard-bristle brush abrade enamel edges, using teeth as tools (opening bottles, tearing tags) transmits abnormal lateral forces, and parafunctional activities like night grinding-seen in roughly 8-31% of adults-apply repetitive loads that extend microcracks.
To reduce progression you can switch to a soft brush and a gentle 45-degree angulation, use fluoride toothpaste to strengthen weakened enamel, stop using teeth as implements, and discuss an occlusal guard if you grind at night; these steps cut mechanical stress and lower the likelihood that a small crack becomes a vertical fracture.
Symptoms of Tooth Cracking
You might see hairline lines (craze lines), chips, or dark discoloration on the enamel while experiencing intermittent sensitivity to cold, sweet, or biting; pain often occurs only when you chew or release pressure. Swelling or a small gum bump near the tooth can appear as infection develops. For example, a molar with a vertical split commonly produces sharp pain on release but little pain at rest.
Physical Indicators
Visible signs include thin vertical lines, flaking enamel, or a portion of the crown that moves slightly when you press. Teeth with cracks may show staining along the fracture or a subtle change in how your bite feels. Sometimes the gum next to the tooth becomes red or forms a localized abscess, and you may notice tenderness when brushing or flossing that specific area.
Associated Pain
Pain can be sharp and fleeting-often triggered by biting hard food or releasing pressure-or dull and lingering when the pulp is inflamed. You may notice heightened sensitivity to cold or sweet that lasts seconds to minutes, and discomfort can radiate into the jaw, ear, or temple, which may make you think the problem lies elsewhere.
Mechanically, movement of cracked fragments transmits stress to the pulp producing sharp bite-related pain; biologically, bacteria can enter the fracture and cause pulpitis, leading to constant throbbing over days. In one reported scenario, intermittent bite pain persisted for weeks before pulp involvement required root canal therapy, showing how episodic symptoms can precede more severe infection.
Risks of Ignoring Small Cracks
If you leave a small crack untreated, daily forces and temperature changes can widen it, turning a minor defect into a fracture, infection, or tooth loss. Thousands of chewing cycles and habits like bruxism (which affects up to 30% of people) accelerate propagation. You may face more complex treatments later-root canal therapy, crowns, or extraction-often increasing chair time and cost compared with early intervention and a bonded restoration.
Progression to Larger Issues
Microcracks act like fault lines: with each bite or grind they can lengthen and deepen, and a sudden event-biting a pit or ice-can convert a hairline fracture into a split tooth. In many cases you’ll notice intermittent sharp pain with chewing before the crack reaches the pulp; once it does, infection risk rises and the tooth can fracture vertically, frequently necessitating extraction rather than repair.
Impact on Overall Oral Health
When a crack exposes dentin or pulp, bacteria gain direct access, increasing your risk of pulpitis, abscess formation, and localized bone loss around the affected root. You might develop persistent sensitivity, swelling, or a draining sinus tract, and adjacent teeth can suffer from altered bite forces and shifting, making comprehensive treatment more involved.
Clinically, a cracked tooth that becomes infected often requires root canal therapy in 1-2 visits followed by a full-coverage crown, but if a vertical root fracture occurs, extraction is commonly the only option. You should also note that untreated infections can lengthen healing time for nearby periodontal tissues; radiographs can reveal bone loss within months, turning a single cracked tooth into a multi-tooth treatment plan.
Preventive Measures
Proper Oral Hygiene
You should brush twice daily for two minutes with fluoride toothpaste, using a soft-bristled brush and replace it every 3 months; floss at least once daily and use interdental brushes for wide spaces. Rinse with a fluoride mouthwash if your dentist recommends it. Avoid chewing ice and hard candies, and wait 30 minutes after acidic drinks before brushing to protect enamel that can hide microcracks.
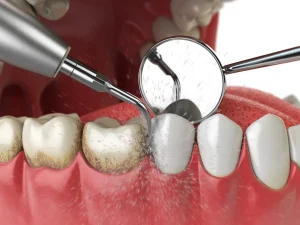
Regular Dental Check-ups
Have professional exams every six months, or more often if you grind teeth or have large restorations; bitewing X-rays every 12-24 months help spot cracks that aren’t visible. Your dentist can use transillumination, intraoral cameras, and dye tests to detect hairline fractures early, then recommend bonding, onlays, or crowns to stop propagation before the pulp is involved.
During a check-up your dentist visually inspects restorations and uses bite tests, percussion, and cold sensitivity to reveal symptomatic cracks; radiographs and magnification document findings. If you report intermittent pain on biting or sensitivity to cold, they may fit an occlusal guard, adjust your bite, or place a protective onlay; patients with bruxism or extensive fillings may be scheduled every 3-4 months to monitor changes and intervene early to avoid root canal or loss.
Treatment Options
You should choose treatment based on crack depth, symptoms, and pulp involvement: options range from bonding and sealants for enamel-only splits to crowns, root canal therapy, or extraction with implant placement for deeper fractures; for example, a hairline enamel crack can be sealed same-day while a crack reaching the pulp often requires root canal plus a crown to prevent infection and restore strength.
Conservative Approaches
When the crack is confined to enamel or outer dentin, you benefit from bonding, glass-ionomer or composite sealants, topical fluoride, occlusal adjustment, and a night guard; bonding and sealants are often completed in one visit, occlusal adjustments may relieve symptoms within 1-2 appointments, and routine radiographic monitoring every 6-12 months lets you catch progression early.
- Dental bonding to seal and stabilize enamel cracks
- Fluoride varnish or sealants for remineralization and protection
- Occlusal adjustment and custom night guard to reduce parafunctional forces
- Periodic monitoring with bitewing or periapical X-rays every 6-12 months
Conservative Approach Details
| Treatment | Use / Key facts |
|---|---|
| Dental bonding | Seals hairline cracks, restores enamel integrity, single-visit |
| Sealants / Fluoride | Promotes remineralization and reduces sensitivity for superficial lesions |
| Night guard / Occlusal adjustment | Reduces peak bite forces and prevents propagation in bruxers |
Advanced Procedures
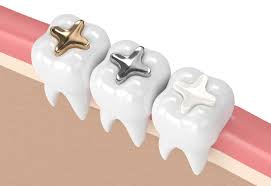
If the crack reaches dentin or the pulp, you’ll likely need definitive care such as a full-coverage crown, root canal therapy (success commonly >85%), or extraction with implant or bridge replacement; crowns often restore function for 5-15 years depending on material, and implants provide a long-term option when the tooth can’t be salvaged.
When a fracture extends below the gum line or into the root, predictability falls and vertical root fractures are frequently non-restorable, leading to extraction; in borderline cases crown lengthening or periodontal surgery may salvage the tooth, while CBCT imaging helps you and your clinician decide between endodontic surgery, restoration, or replacement with an implant (long-term success >90%).
- Full-coverage crown to protect and redistribute occlusal forces
- Root canal therapy to remove infected pulp and preserve the tooth
- Endodontic surgery (apicoectomy) for localized root issues
- Crown lengthening or periodontal surgery to expose restorative margin
- Extraction followed by implant or fixed bridge when non-restorable
Advanced Procedure Details
| Procedure | When used / Key facts |
|---|---|
| Full-coverage crown | Protects weakened tooth; lifespan ~5-15 years depending on material |
| Root canal therapy | Removes infected pulp; typical success rates exceed 85% |
| Extraction & implant | Used when tooth is non-restorable; implants show long-term success >90% |
To wrap up
With this in mind, even tiny cracks in your teeth can allow bacteria and stress to penetrate enamel, leading to decay, infection, sensitivity, and progressive structural failure; untreated microfractures often expand under chewing forces, complicate treatment, and can necessitate root canals or extractions, so you should seek prompt diagnosis and protective treatment to preserve function and avoid more invasive, costly procedures.